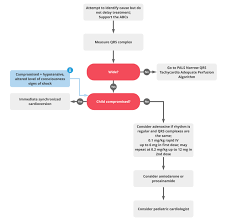
During medical emergencies Advanced Cardiac Life Support (ACLS) is essential. This offers procedures to address cardiac arrests, strokes and various urgent health crises. However, when it comes to children, the standard ACLS procedures require adjustments.
The anatomy and physiological responses of pediatric patients differ significantly from adults, making a specialized approach essential. In this blog post we will explore how the Step-by-step ACLS algorithm can be tailored for patients. Additionally, we will highlight the adjustments and important factors to increase the survival of the young patients in critical emergencies.
Through examining these modifications we aim to provide healthcare practitioners with insights into the methods for implementing ACLS protocols in children. This will help ensure that they receive efficient care, in urgent situations.
Understanding ACLS Algorithm for Pediatric Patients
The Advanced Cardiac Life Support (ACLS) algorithm is a guide for healthcare professionals to handle severe cardiac emergencies. The primary objectives involve reinstating a heartbeat and maintaining blood circulation to essential organs. The process entails identifying arrest, administering CPR and utilizing medications and defibrillation when necessary.
When implementing the ACLS protocol, for patients it is crucial to take into account physiological variances, between children and adults.
- Smaller Airway Size: Children have smaller airways compared to adults, making them more prone to obstruction. This necessitates adjustments in airway management techniques to ensure they are effective and do not cause harm.
- Higher Metabolic Rate: Pediatric patients have a higher metabolic rate, meaning their oxygen needs are greater. The ACLS algorithm must account for this by emphasizing quick and efficient oxygen delivery.
- Heart Rate and Blood Pressure Variability: The normal ranges for heart rate and blood pressure vary widely in children, depending on their age. Recognizing what is normal for the specific age group is crucial in identifying and treating cardiac emergencies.
- Differences in Cardiac Arrest Causes: In children, cardiac arrest is often the result of respiratory failure or shock rather than a primary cardiac event. This difference affects the approach to treatment, prioritizing airway management and circulation support.
Tailoring cardiac life support to the pediatric population is vital for improving outcomes. Recognizing and adapting to the unique physiological needs of children ensures that the ACLS algorithm can be applied effectively, offering the best chance for recovery in these critical situations.
Key Modifications in the Pediatric ACLS Algorithm
In adapting the Advanced Cardiac Life Support (ACLS) algorithm for pediatric patients, several key modifications are essential to address their unique needs:
- Airway Management: The airway anatomy of children is notably different from that of adults. Their airways are smaller and more easily obstructed. This reality demands specific strategies for opening and maintaining the airway, ensuring that ventilation is both effective and gentle to prevent injury.
- Drug Dosages: The dosage of medications in the ACLS protocol for children must be carefully adjusted based on their weight. This precision is crucial because the same dose given to adults can have vastly different effects in the smaller bodies of children. Accurate dosing ensures the effectiveness of the drugs while minimizing the risk of adverse effects.
- Defibrillation: For pediatric patients, the energy levels used in defibrillation are lower than those for adults. Additionally, pediatric paddles or pads are utilized to suit their smaller body size. These adjustments are vital to ensure that defibrillation is both safe and effective in correcting life-threatening cardiac rhythms without causing harm to the child’s more delicate body.
- CPR Technique: The technique for performing CPR on infants and children also differs. The depth of chest compressions and the rate at which they are administered are adjusted to match the size and physiology of younger patients. These modifications are designed to optimize blood flow during cardiac arrest while minimizing the risk of injury.
These modifications to the ACLS algorithm are critical for providing effective and safe emergency cardiac care to pediatric patients. Tailoring the approach to their specific physiological characteristics significantly improves the chances of a successful outcome.
Special Considerations for Pediatric Patients
Dealing with pediatric emergencies requires not only medical expertise but also a deep understanding of the psychological aspects involved. The emotional impact on the healthcare team can be significant, as treating young patients in critical conditions is both challenging and distressing. Recognizing and managing these emotions are crucial for maintaining the team’s focus and effectiveness during emergencies.
Communication with the child’s family is another vital consideration. Families are often overwhelmed with fear and anxiety during such critical times. Healthcare professionals must communicate clearly, compassionately, and honestly, providing updates and explanations in a way that is understandable and respectful. This approach helps to build trust and eases the emotional burden on the family.
The role of Pediatric Advanced Life Support (PALS) training is indispensable in preparing healthcare professionals for these situations. PALS training equips them with the specific skills and knowledge needed to effectively respond to cardiac emergencies in children. It also addresses the unique psychological and communication challenges that arise when caring for pediatric patients. Through this specialized training, healthcare providers are better prepared to offer high-quality care, ensuring both the medical and emotional needs of the child and their family are met.
Conclusion
When adapting the Step-by-step ACLS algorithm for pediatric patients it’s evident that making adjustments is crucial. The distinct physiological variances between kids and grown ups require these modifications to guarantee that life saving treatments work well and are safe for individuals. Important changes involve customized airway handling, accurate medication doses, adjusted defibrillation methods and modified CPR approaches, all aimed at addressing the requirements of children’s frames and faster metabolism.
Furthermore, the emotional and psychological aspects of pediatric emergency care cannot be overlooked. Effective communication with the child’s family and the emotional support for healthcare teams are pivotal. Training in Pediatric Advanced Life Support (PALS) is essential as it provides professionals with the skills to handle the emotional complexities that come with pediatric emergencies.
The main objective of these adjustments and focused training programs is to enhance survival rates and results for patients dealing with emergencies. By ensuring that healthcare providers are adequately trained to implement these tailored ACLS protocols we can deliver care to children, in situations.